Understanding Medicare Coverage for CPAP Treatment in Sleep Apnea Management
Wondering if Medicare covers CPAP treatment for sleep apnea? Discover how Medicare policies might include CPAP therapy and the criteria involved. Medicare’s coverage for CPAP treatment hinges on specific qualifications, and understanding these can help manage sleep apnea effectively.
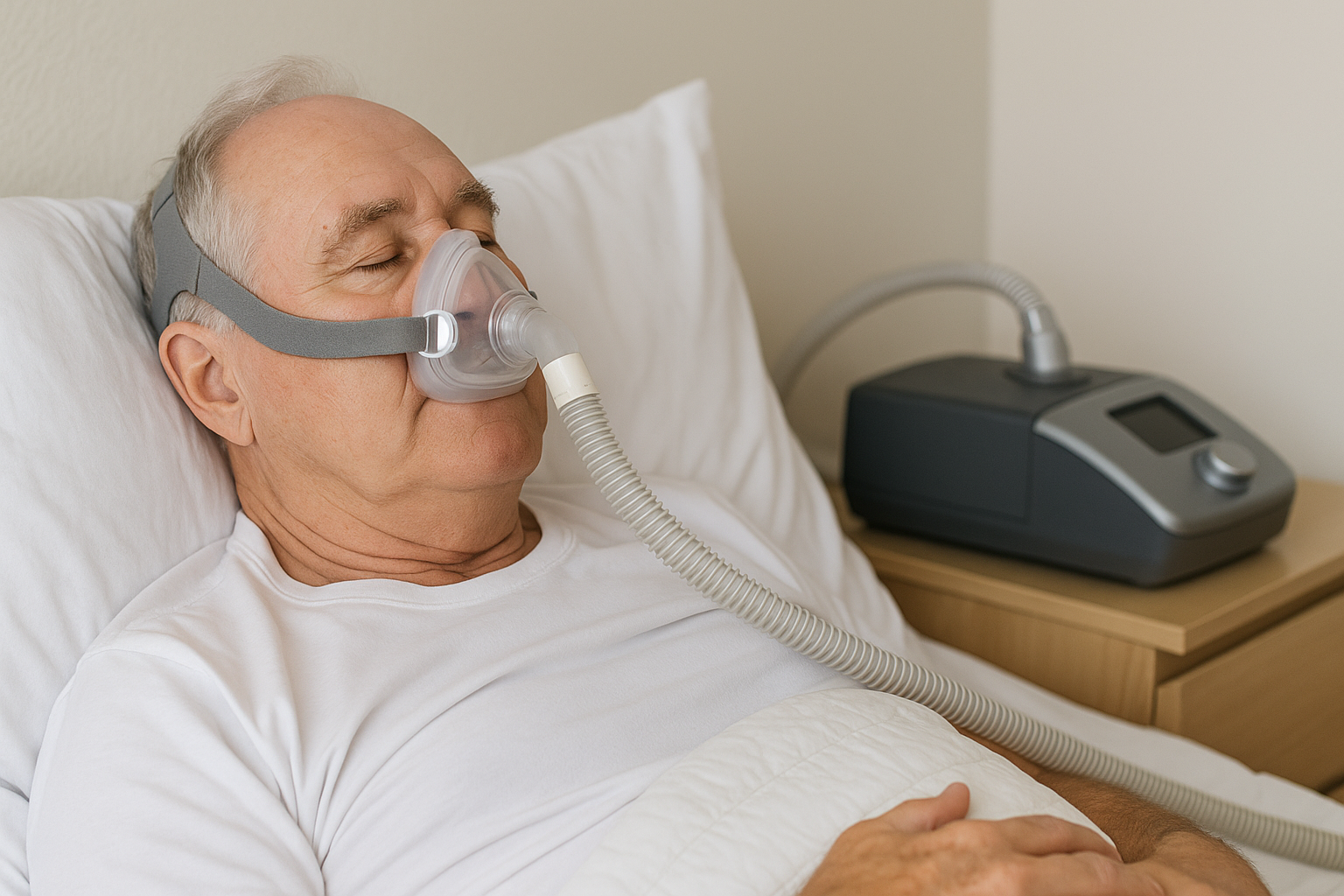
Understanding Medicare Coverage for CPAP Treatment
For many individuals diagnosed with sleep apnea, Continuous Positive Airway Pressure (CPAP) therapy is a crucial component of managing their condition. However, one common question is, "Does Medicare cover CPAP treatment for sleep apnea?" This article aims to unravel the nuances of Medicare coverage for CPAP therapy, providing you with comprehensive insights into what to expect, how to qualify, and how to make the most of your Medicare benefits.
What is Sleep Apnea and CPAP Therapy?
Sleep apnea is a potentially serious sleep disorder where breathing repeatedly stops and starts. The most common form is obstructive sleep apnea (OSA), which occurs when throat muscles intermittently relax and block your airway during sleep. This can severely impact your sleep quality and overall health if left untreated.
CPAP therapy involves using a machine that delivers a steady stream of air through a mask, keeping airways open during sleep. This treatment is highly effective, improving sleep quality and reducing associated health risks like high blood pressure, heart disease, and more.
Medicare Coverage for CPAP Equipment and Services
Medicare primarily consists of two parts relevant to most CPAP users: Part B (Medical Insurance) and Part C (Medicare Advantage). Eligibility for coverage typically requires a formal diagnosis of sleep apnea following a sleep study conducted at a sleep center or through in-home testing.
Medicare Part B
Under Medicare Part B, CPAP machines and related equipment are covered as durable medical equipment (DME). This coverage includes the CPAP device, masks, and necessary accessories such as tubing and filters. To qualify:
- You must be officially diagnosed with obstructive sleep apnea.
- A healthcare provider and supplier must be enrolled in Medicare.
Once you qualify, Medicare typically covers up to 80% of the Medicare-approved amount for the machine and supplies, while you are responsible for the remaining 20%, unless you have additional coverage such as Medigap.
Medicare Advantage (Part C)
Medicare Advantage plans, offered by private insurance companies, must cover everything that Original Medicare (Part A and Part B) covers, thus including CPAP treatment. However, the plans may have varied rules, costs, and clinicians within their network.
It’s essential to consult with your Medicare Advantage plan provider to understand specifics, such as pre-authorization requirements and the network of available DME suppliers.
How to Obtain CPAP Equipment with Medicare
To procure a CPAP machine through Medicare, follow these steps:
- Diagnosis: Obtain a formal diagnosis from a sleep specialist after a polysomnography test or home sleep apnea test.
- Prescription: Get a prescription from your doctor detailing the specific CPAP equipment needed.
- Supplier Selection: Choose a Medicare-enrolled DME supplier. Use the Medicare Supplier Directory to find a qualified supplier near you.
- Rental Period: Medicare initially covers CPAP machine rental for a 13-month trial period. After successful adherence and effectiveness, ownership of the machine typically transitions to you.
What Does the Coverage Include?
Medicare’s coverage includes several vital components:
- CPAP Machines: Basic CPAP apparatus designed specifically for your breathing needs.
- Masks and Headgear: Designed for comfort and an effective seal, often including nasal masks, nasal pillows, or full face masks.
- Tubing and Filters: Necessary for connecting the mask to the machine and ensuring clean air is circulated.
- Humidifiers: Integrated in some CPAP machines to moisten the air and prevent dryness.
The frequency of replacements and maintenance parts may vary, but Medicare typically allows mask replacement every three months and filter replacement every month, depending on individual circumstances and supplier policies.
Recent Developments and Statistics in CPAP Usage
According to a 2026 report from the National Sleep Foundation, the prevalence of diagnosed sleep apnea has increased by about 12% in recent years, emphasizing the growing demand for treatment options like CPAP therapy. Simultaneously, studies show that usage compliance among patients has improved, largely due to greater awareness and easier access to treatment solutions.
Managing Costs Beyond Medicare Coverage
Besides the 20% coinsurance, individuals with high-deductible plans may incur significant upfront costs until they meet their deductibles. Consider these strategies to manage expenses:
- Look into supplemental insurance like Medigap, which can cover the remaining costs associated with CPAP therapy beyond the Medicare-approved amount.
- Check if your Medicare Advantage plan offers extra benefits that might lessen out-of-pocket expenses for CPAP equipment and supplies.
Conclusion
Understanding the scope of Medicare coverage for CPAP treatment can optimize the management of your sleep apnea, improving both your health and financial planning. For further assistance and tailored advice, consult with your healthcare provider or connect with your local Medicare office to gain a comprehensive view of your coverage options.
With the right information and resources, you can successfully navigate Medicare's processes to get the right CPAP treatment that plays a pivotal role in ensuring restful, healthier sleep.