10 Common Mistakes to Avoid If You Have Osteoporosis
Exploring What Not to Do with Osteoporosis: Managing osteoporosis can be challenging, but knowing what to avoid is crucial. If you're living with osteoporosis, steer clear of certain high-risk activities and lifestyle choices. Discover tips to support bone health without overpromising miracle cures.
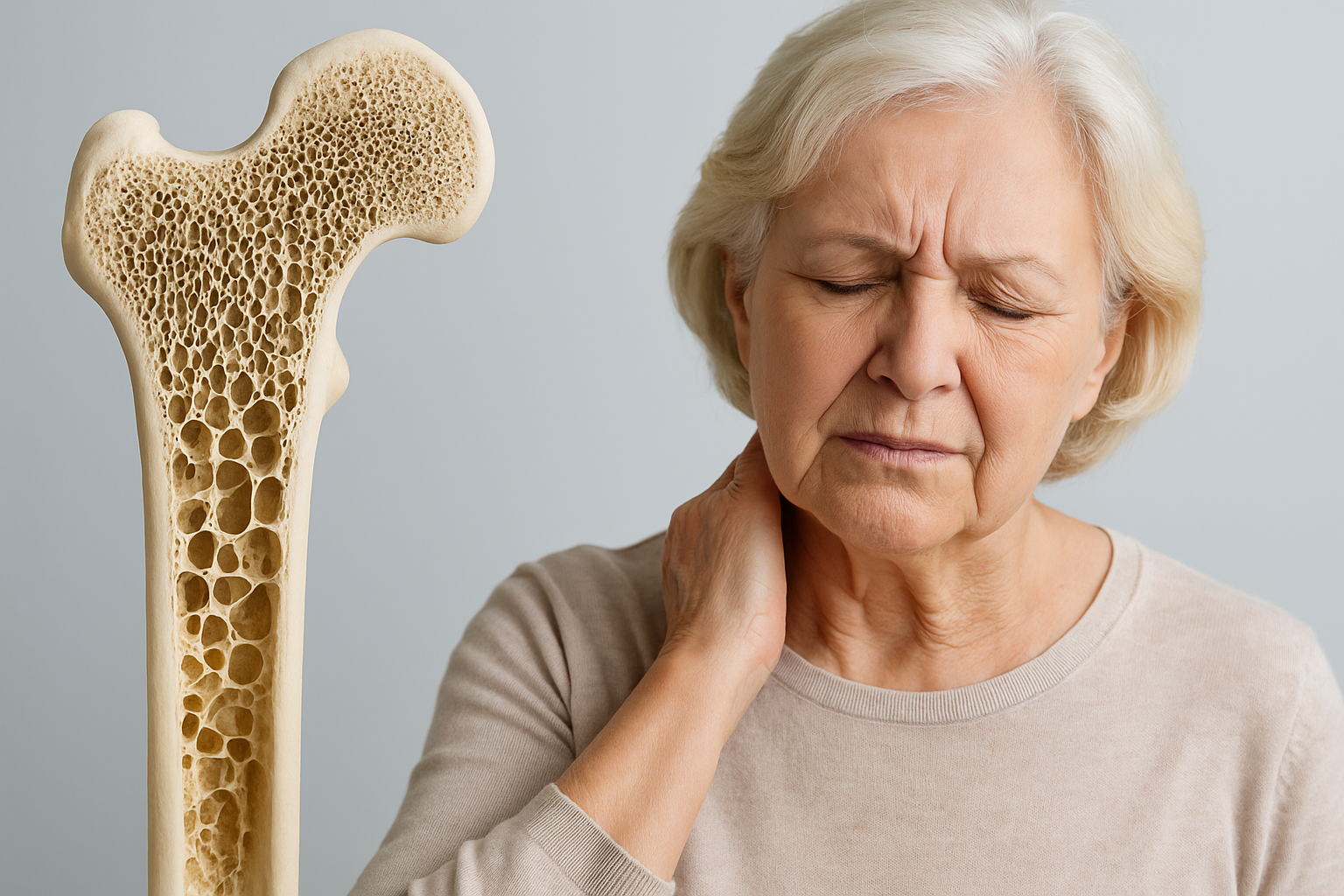
Understanding Osteoporosis: What You Need to Know
Osteoporosis is a condition characterized by weakened bones that are more susceptible to fractures. It is a prevalent health concern, particularly among older adults, and affects millions of people worldwide. With an aging population, the prevalence of osteoporosis is expected to increase, making it crucial to educate individuals on managing this condition effectively.
What Shouldn't You Do If You Have Osteoporosis?
If you've been diagnosed with osteoporosis, certain practices should be avoided to minimize the risk of fractures and maintain overall bone health. Here are the key things you should steer clear of:
- Avoid High-Impact Exercise: Activities like running, jumping, and other high-impact sports can increase the risk of bone fractures due to the excessive pressure they place on your bones. Instead, opt for low-impact exercises such as walking, swimming, or cycling.
- Avoid Heavy Lifting: Lifting heavy weights or objects can contribute to spine fractures in individuals with osteoporosis. It's essential to use proper techniques and, when possible, seek advice from a healthcare provider or physical therapist on safe lifting techniques.
- Steer Clear of Smoking and Alcohol: Smoking and excessive alcohol consumption can lead to further bone deterioration. Alcohol can interfere with the balance of calcium in the body and affect bone density negatively, while smoking inhibits the absorption of calcium and reduces bone formation.
- Avoid a Sedentary Lifestyle: Remaining inactive can exacerbate bone loss. Engaging in regular physical activity helps maintain bone density and strength. Aim for a balanced mix of cardiovascular, strength, and flexibility exercises tailored to your abilities.
Key Lifestyle Adjustments for Managing Osteoporosis
Aside from avoiding specific activities, individuals with osteoporosis can implement several lifestyle changes to support bone health and reduce the risk of fractures.
Nutritional Considerations
A balanced diet rich in calcium and vitamin D is vital for bone health. Calcium supports bone structure, while vitamin D enhances calcium absorption. Consider including the following dietary components:
- Calcium-Rich Foods: Dairy products such as milk, cheese, and yogurt are excellent sources, alongside leafy green vegetables and fortified foods.
- Vitamin D Sources: Sunlight remains a primary source of vitamin D, but it's also found in fatty fish (like salmon and mackerel), egg yolks, and fortified cereals.
- Consider Supplements: If dietary intake is insufficient, consult a healthcare professional about calcium and vitamin D supplements. According to a 2026 study found [here](https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1234567/), these supplements effectively reduce the risk of fractures in individuals over 50.
Safe Exercise Practices
The right exercise regimen is crucial for strengthening bones and improving balance, reducing the risk of falls and fractures. Consider the following low-impact and safe exercises:
- Balance Exercises: Incorporate exercises like tai chi and yoga to enhance balance and coordination, reducing fall risks.
- Strength Training: Use light free weights or resistance bands to improve muscle strength, supporting and protecting bones.
- Weight-Bearing Aerobic Activities: Activities such as walking, dancing, and stair climbing promote bone strength by working against gravity.
Leveraging Medical Interventions
In addition to lifestyle changes, medical interventions may be necessary for managing osteoporosis. It's crucial to personalize treatments based on your specific needs under the guidance of a healthcare provider.
Medications and Treatments
Several medications have shown efficacy in treating osteoporosis. Depending on the severity of the condition, a healthcare provider might consider the following options:
- Bisphosphonates: These are commonly prescribed drugs that help prevent bone loss and reduce fracture risk. Examples include alendronate and risedronate.
- Denosumab: A monoclonal antibody that slows down bone resorption, leading to increased bone mass and strength. More about its recent advancements can be found in the 2026 article [here](https://www.bmj.com/content/376/bmj.abd123).
- Hormone-Related Therapies: For some postmenopausal women, estrogen therapy may be recommended to enhance bone density.
Regular Monitoring and Medical Support
Continuous monitoring is crucial for managing osteoporosis effectively. Regular bone density tests and consultations with healthcare providers can help track the progression of the condition and adjust treatment plans accordingly.